
Achilles Tendon Treatment in Brooklyn for Runners & Active Adults
At Form & Function Chiropractic, treatment begins with precise tissue diagnosis to determine whether symptoms involve Achilles tendinopathy, partial tendon injury, calf overload, or related conditions.
Achilles pain can limit walking, running, and performance — and often becomes persistent if the underlying cause isn’t addressed.
Treatment focuses on:
reducing pain
restoring tendon capacity
preventing recurrence
Using a combination of regenerative therapy and load-based rehabilitation.
Because pain relief isn’t enough — your tendon has to be strong enough to handle load again.

What Is Achilles Tendinopathy?
The Achilles tendon connects the calf muscles to the heel and plays a critical role in walking, running, and jumping.
Achilles tendinopathy develops when the tendon becomes overloaded, irritated, or degenerative due to repetitive stress.
This is one of the most common overuse injuries in runners and active individuals.
What is the difference between insertional and mid-portion Achilles tendinopathy?
Achilles tendinopathy is commonly divided into two types based on location:
Mid-Portion Achilles Tendinopathy
occurs 2–6 cm above the heel bone
more common in runners
typically related to repetitive loading and overuse
often responds well to progressive loading programs
Insertional Achilles Tendinopathy
occurs where the tendon attaches to the heel (calcaneus)
often more sensitive to compression
aggravated by:
uphill running
deep calf stretching
certain footwear
requires modification of loading strategies (not treated the same as mid-portion)
Correct diagnosis matters. This is where Clarius MSK Diagnostic Ultrasound can help confirm the exact location and guide treatment
Treating insertional Achilles pain like mid-portion tendinopathy can actually make symptoms worse.
What Causes Achilles Tendon Pain?
Achilles tendon pain is typically a load management problem — not just inflammation.
Common contributors include:
sudden increases in running or training volume
tight or overloaded calf muscles
poor ankle mobility
inefficient running mechanics
inadequate strength or tendon capacity
The Achilles can experience forces up to 10–12x body weight during running, making it highly sensitive to load errors.
LOAD > CAPACITY = PAIN

Common Symptoms of Achilles Tendinopathy
pain or stiffness in the back of the heel
pain at the start of activity that may improve, then return
morning stiffness
tenderness or thickening of the tendon
pain with running, jumping, or push-off
Why Achilles Tendon Pain Keeps Coming Back
Most cases recur because the tendon feels better before it is actually stronger.
Common reasons include:
returning to running too quickly
not restoring full calf strength
ignoring tendon load capacity
relying only on rest or passive care
If tendon capacity is not rebuilt, the same stress will reproduce the injury.
Why Rest, Stretching, and Passive Care Aren’t Enough
Traditional approaches often focus on:
rest
stretching
anti-inflammatory strategies
While these may reduce symptoms temporarily, they do not restore tendon capacity.
Evidence consistently shows that progressive loading is the foundation of tendon recovery.
Conditions That Can Mimic Achilles Tendon Pain
Achilles region pain may also involve:
retrocalcaneal bursitis
nerve irritation
Differentiating these conditions ensures targeted therapy rather than generic treatment.
How We Treat Achilles Tendon Pain in Brooklyn
Treatment is built around a multimodal regenerative and load-based approach:
reduce pain and irritation
improve tendon healing response
restore calf strength and tendon capacity
improve movement mechanics
safely return to running and activity
Regenerative Therapy & Advanced Modalities
Regenerative therapies are used to reduce pain, improve tendon response, and accelerate recovery — allowing the tendon to better tolerate progressive loading.
These are not standalone treatments — they are integrated into a structured rehabilitation plan.
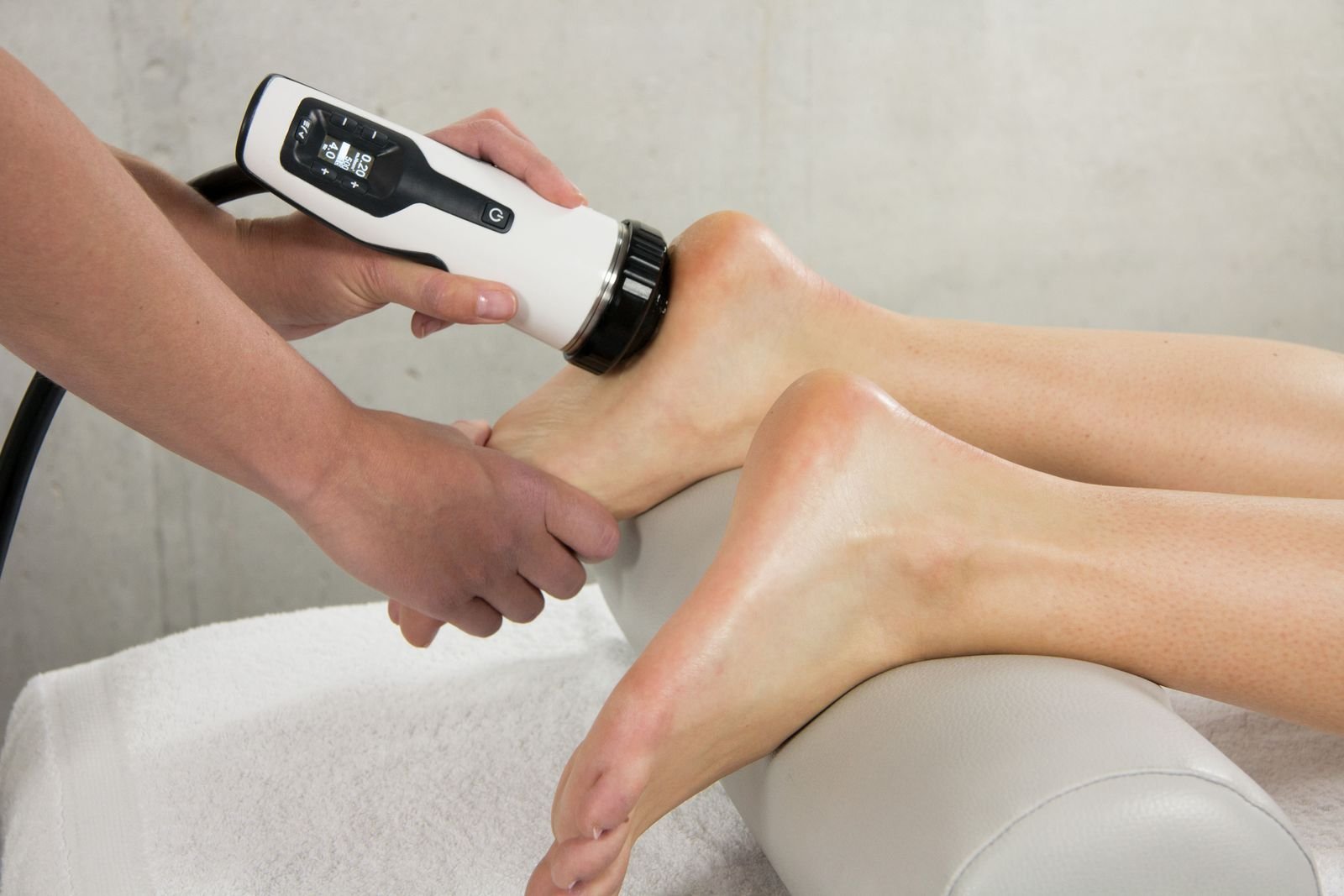
Shockwave Therapy (Focused & Radial)
Shockwave therapy is used for:
reduce pain sensitivity
stimulate tendon remodeling
improve local circulation
Focused shockwave targets deeper tendon structures, while radial pressure wave therapy addresses surrounding tissue and overload patterns.
Used extensively for chronic Achilles tendinopathy.
EMTT (Extracorporeal Magnetotransduction Therapy)
EMTT is a high-energy electromagnetic therapy that works at the cellular level to improve how injured tissue heals and responds to load.
improves cellular activity and energy production
supports collagen remodeling and tendon repair
reduces inflammation and pain sensitivity
enhances tissue response to rehabilitation
chronic Achilles issues are often a failed healing response, not just inflammation.
EMTT helps “re-activate” the tendon’s ability to adapt and recover — especially in stubborn or long-standing cases.
Laser Therapy (Photobiomodulation)
Laser therapy helps:
reduce inflammation
improve cellular energy production
support recovery
Functional Range Conditioning (FRC®) & Load-Based Rehabilitation
Long-term recovery depends on rebuilding tendon capacity.
(FRC®) includes:
calf strengthening (eccentric + progressive loading)
ankle mobility and control
foot and lower limb stability
movement retraining
Progressive loading programs are strongly supported in Achilles rehab research.
Return-to-Run Progression
Returning to running too quickly is one of the most common causes of recurrence.
A structured return-to-run plan ensures the tendon adapts safely to increasing load and intensity.
For runners and active individuals, Achilles tendon load is strongly influenced by cadence, stride mechanics, terrain demands, and training progression.
Biomechanical running analysis may be incorporated when appropriate.
👉 Learn more about
Running Gait Analysis & Performance Assessment in Brooklyn
Objective assessment helps guide:
safe return-to-running progression
cadence and stride modification
workload planning
injury risk reduction strategies
Running Biomechanics & Return-to-Running Strategy


Pain Reduction Is Not the Same as Tendon Recovery
Pain may decrease before the tendon is ready for full load.
True recovery means:
strength is restored
load is tolerated
movement is efficient
How Long Does Achilles Tendon Recovery Take?
Most cases improve within:
4–8 weeks for mild cases
longer for chronic or recurrent issues
Recovery depends heavily on load management and consistency.
When Should You Seek Treatment?
You should seek care if:
pain persists beyond 1–2 weeks
symptoms worsen with activity
stiffness is increasing
running or walking is limited
Frequently Asked Questions About Achilles Tendon Pain
-
There is no true shortcut.
The most effective approach combines:
load management
progressive calf strengthening (not stretching, which can aggravate symptoms)
Rest alone may reduce pain temporarily, but it does not restore tendon capacity — which is why symptoms often return.
-
Achilles tendinopathy is divided into two types based on location.
Mid-portion tendinopathy:
occurs 2–6 cm above the heel
more common in runners
responds well to progressive loading
Insertional tendinopathy:
occurs at the heel attachment
more sensitive to compression
aggravated by deep stretching and uphill activity
These conditions require different treatment strategies.
-
Not always.
In many cases, running is modified rather than stopped completely, depending on pain levels and tendon tolerance.
The goal is to:
reduce excessive load
maintain activity where possible
progress safely
-
Yes — they are one of the most effective treatments.
Progressive calf loading helps:
strengthen the tendon
improve load tolerance
reduce long-term pain
They must be progressed properly based on tolerance — not done randomly.
-
Because pain improves before the tendon has fully recovered.
This leads to:
returning to activity too early
reloading tissue that isn’t ready
Pain relief is not the same as tendon recovery.
-
Yes — especially in chronic or persistent cases.
Shockwave therapy can:
reduce pain sensitivity
stimulate tendon remodeling
improve healing response
It is most effective when combined with a structured loading program.
-
EMTT is a high-energy electromagnetic therapy that works at the cellular level.
It helps:
improve tissue healing response
support tendon remodeling
enhance recovery in stubborn cases
It is often combined with shockwave therapy for better results.
-
Not always — but when needed, it can be done in-office.
Using Clarius MSK diagnostic ultrasound, the tendon can be assessed in real time for:
thickening
degeneration
partial injury
This helps guide more precise treatment.
-
Most cases improve within:
4–8 weeks for mild to moderate cases
longer for chronic or recurrent issues
Recovery depends on:
consistency
proper loading
avoiding early return to full activity
-
Yes — if overload continues without restoring tendon capacity.
Persistent symptoms increase the risk of:
partial tearing
full rupture
Early, structured treatment significantly reduces this risk.
-
Most approaches focus only on reducing pain.
Our approach focuses on:
precise tissue and loading diagnosis
biomechanical movement and running analysis
integration of shockwave therapy, EMTT, and laser therapy
return-to-sport and long-term injury prevention strategies
Collaborative, Not Isolated Care
Podiatrists play an important role in evaluating foot and ankle conditions — particularly when imaging, orthotics, injections, or surgical consultation are needed.
Many patients are referred for rehabilitation after initial podiatric evaluation when symptoms persist or when a structured, load-based approach is required.
If clinical findings suggest that podiatric or surgical care is more appropriate, referral is recommended.
Get Back to Running Without Achilles Pain
Achilles pain rarely improves with rest alone. It requires the right combination of precise diagnosis, regenerative therapy, and progressive loading to restore tendon capacity and reduce recurrence.
